AGES Radar for Infectious Diseases – 12 March 2026
Summary
Following a significant decline in influenza activity, the flu outbreak in Austria has come to an end, with only sporadic cases now being detected. The number of RSV cases remains high, whilst SARS-CoV-2 is circulating at low levels.
On 9 March, an update on Cereulid in infant formula was published on the AGES website. In Austria, 13 cases of Cereulid infection in infants had been reported in the epidemiological reporting system as of 4 March 2026.
Following England, India has now also reported a case of the recombinant Mpox virus from clades Ib and IIb. In Austria, cases of Mpox from clade Ib have been recorded for the first time since February.
Since the end of 2025, there has been an increase in cases of Chikungunya virus disease in Austria and other EU Member States among travellers returning from the Seychelles.
What do hares, ticks and humans have in common? In this month’s feature, we take a closer look at the bacterium Francisella tularensis and the disease it causes, tularemia.
In the news: Chile is the second country in the world to be officially declared leprosy-free. Denmark is the first EU country to have eliminated vertical transmission of HIV and syphilis. The annual reports of the National Reference Centres for Pneumococcal and Legionella Infections, as well as the Mosquito Alert annual report, have been published. Germany reported a case of rabies in an imported dog with a contact dog in Austria; measures have been initiated.
The flu outbreak in Austria has come to an end. Following a steady decline in influenza detections in the sentinel system over recent weeks, the positivity rate fell below the epidemiological threshold of 10% in calendar week (CW) 8. By early March, only isolated cases were being detected. The AGES wastewater monitoring programme now shows no further evidence of influenza viruses.
The influenza detections were almost exclusively attributable to influenza A, subtypes A(H3N2) and A(H1N1). Influenza B was detected in only 1% of all samples. Hospital admissions for influenza have been declining since the start of the year: at the beginning of January, 863 admissions per week were recorded in general wards; by the end of February, this figure had fallen to just 49. As corrections and late reports are to be expected, the data may still change.
In most countries of the European Union and the European Economic Area (EU/EEA), influenza circulation is declining, as are hospital admissions. People aged 65 and over account for the majority of admissions. A(H3) remains the dominant subtype, followed by A(H1)pdm09.
The best preventive measure against severe influenza is the annual flu vaccination. In Austria, vaccination against influenza (true flu) is recommended from the age of 6 months and is available free of charge to all age groups under the public vaccination programme. Vaccination is particularly important for people at risk of severe illness and their close contacts/household members, as well as for those who are at increased risk of infection due to their living circumstances (including pregnant women) or occupation. A nasal vaccine is available specifically for children. Ideally, the influenza vaccination should be administered in mid-October or November, before the flu season begins. Details can be found at www.impfen.gv.at/influenza and in the current Austrian Vaccination Schedule 2025/2026.
In episode 003 – Influenza & Co: How do I navigate the flu season safely? of the AGES podcast “Mut zum Risiko”, infectious disease epidemiologist Fiona Költringer explains what the flu is all about and how best to protect yourself against it.
After England identified a new recombinant mpox virus (MPXV) in a person in December, India also reported a mpox case in January involving a recombinant MPXV from clades Ib and IIb. Analysis of the viral genomes shows that the two individuals contracted the same recombinant viral strain several weeks apart. This suggests that there may be further, unknown cases. Both cases have a travel history, albeit to different locations. The English case had been travelling in South-East Asia in October 2025, whilst the Indian case developed symptoms in September 2025 after visiting the Arabian Peninsula.
Contact tracing has been completed: to date, no secondary transmissions from these cases or further cases of this recombinant strain have been documented in other parts of the world. There is also no evidence that this recombinant strain is more transmissible or causes more severe illness. Both cases presented a similar clinical picture to that observed in other previously known clades. Neither patient developed severe illness.
Recombination is a known natural process that can occur when two related viruses infecting the same person exchange genetic material, thereby creating a new virus.
Since 23 May 2022, a total of 393 Mpox cases have been recorded in Austria. In 2026, six cases of mpox have been reported so far, including five cases of clade Ib for the first time in February and March. (As of 09/03/2026) Since the start of the outbreak in 2022, only cases of clade II had previously been detected in Austria.
Mpox is mainly transmitted through close (sexual) contact, particularly through direct contact with skin lesions (blisters, scabs, etc.). The available Mpox vaccine is recommended exclusively for people at risk, such as those with high-risk behaviour (people with frequently changing sexual partners). To prevent infection following contact with a person with Mpox, post-exposure vaccination is available and is recommended regardless of age. The vaccine is not available on the open market in Austria and is offered free of charge only at selected vaccination centres in the federal states.
Communicable Disease Threats Report, 14–20 February 2026, Week 8
Mpox: recombinant virus with genomic elements of clades Ib and IIb – Global situation
Mpox | Vaccination simply protects.
It’s that time of year again: we’re seeing the first warmer days, spring is just around the corner – and so are the odd tick or two. Although ticks can now be active all year round in Austria, their activity increases from March onwards.
Vector monitoring plays an important role at AGES and is being gradually expanded. As part of EU projects such as RAISE – Reinforcing Austrian Integrated Surveillance and Epidemiology – and United for Surveillance (U4S), ticks are tested for various pathogens, including Francisella tularensis, the pathogen responsible for tularemia.
Key facts about the pathogen and the disease
Tularemia, a notifiable infectious disease, is caused by the bacterium Francisella tularensis. Francisella tularensis is found in a wide variety of animals (hares, ticks, mosquitoes, etc.), in humans and freely in the environment.
One of the characteristics of the bacterium is that
- it is highly resistant: it can survive in the environment for weeks or months and thus cause infection in humans through contact with contaminated water or soil
- it is highly infectious: even low concentrations of the bacterium are sufficient to trigger infection in humans
- it is not only transmitted via animals and vectors, but can also be inhaled via the air (bacteria attached to airborne particles), giving it a high bioterrorism potential
All very good reasons to take a closer look at it.
Francisella tularensis has several subtypes, which have varying global distributions. It is primarily found in the northern hemisphere and does not normally occur in the tropics or the southern hemisphere. Four subspecies are currently known:
- Francisella tularensis subsp. tularensis (Type A), the most virulent subspecies found only in North America, which is primarily found in lagomorphs and is mainly transmitted to humans via ticks or biting flies, or through direct contact with infected animals
- Francisella tularensis subsp. holarctica (Type B), the most widespread subspecies. It is found mainly in aquatic rodents (beavers, muskrats) and voles in North America, as well as in lagomorphs (hares) and rodents in Eurasia, and causes less severe symptoms in humans than Type A; in Austria, only this Type B is prevalent
- Francisella tularensis subsp. mediasiatica, found primarily in Central Asia
- Francisella tularensis subsp. novicida, the least virulent subspecies
F. tularensis occurs in our latitudes mainly in lagomorphs and rodents. However, the pathogen has also been found in a wide variety of other mammals, as well as in birds, fish, amphibians, arthropods and protozoa. Blood-sucking arthropods, such as mosquitoes and ticks, play an important role both in the maintenance of F. tularensis in the wild and in the transmission of the disease caused by F. tularensis. Tularemia is a zoonosis, i.e. a disease that can be transmitted from animals to humans. Mosquitoes and ticks act not only as natural reservoirs for the bacteria but also as vectors.
The most common routes of transmission of F. tularensis to humans are:
- Direct contact with infected animals, particularly hares. Infection can occur through skin or mucous membrane contact with infectious animal material. Inhalation of infectious dust – for example from soil, straw, hay or animal hides (e.g. when skinning hares) – is also possible
- Stings or bites from arthropods, particularly ticks or mosquitoes
- Contact with contaminated water or soil
Human-to-human transmission has not yet been reported.
In Europe, only the subtype Francisella tularensis subsp. holarctica (type B) causes the disease tularemia. To date, two life cycles of type B have been described. In the terrestrial cycle, the pathogen is primarily spread via hares, small rodents and ticks. Humans usually become infected through contact with infected animals, their meat or through tick bites. Cases tend to occur sporadically or in small outbreaks during the hunting season and result in febrile symptoms, which are frequently accompanied by skin lesions (ulceroglandular form) or swollen lymph nodes (glandular form). In the aquatic cycle, however, the pathogen circulates in aquatic ecosystems and semi-aquatic rodents (e.g. beavers). Transmission to humans occurs primarily via contaminated drinking water or mosquito bites. This often leads to major summer outbreaks, typically involving diseases of the mouth and throat (oropharyngeal form) or – in the case of mosquitoes – also ulceroglandular forms (Maurin & Gyuranecz, 2016).
Severe forms involving the lungs (pulmonary form) can occur in Europe in both cycles, e.g. following inhalation of pathogen-containing dust or water droplets. Table 1 compares the two life cycles:
In humans, the incubation period is usually around 3 to 5 days, but can last up to 14 days. Tularemia presents with a wide variety of clinical presentations. Common symptoms include fever, headache, aching limbs and painful swelling of the regional lymph nodes. After a few days, localised ulcers may also develop at the site where the pathogen entered the body. Depending on the type and route of transmission of the infection, the course of the disease may vary, with additional symptoms such as sore throat, vomiting, diarrhoea, pneumonia or abdominal pain.
Timely antibiotic treatment is highly effective; there is currently no vaccine available.
In particular, groups of people who spend a lot of time in the great outdoors – such as the rural population, hunters, forestry workers, etc. – are at increased risk of coming into contact with F. tularensis. As there is no vaccine, the following measures are recommended:
- Use insect repellent
- Wear gloves when handling sick or dead animals. Recently killed sick hares or those found dead must not be skinned, but should only be touched with gloves and immediately packed securely
- Avoid mowing over dead animals
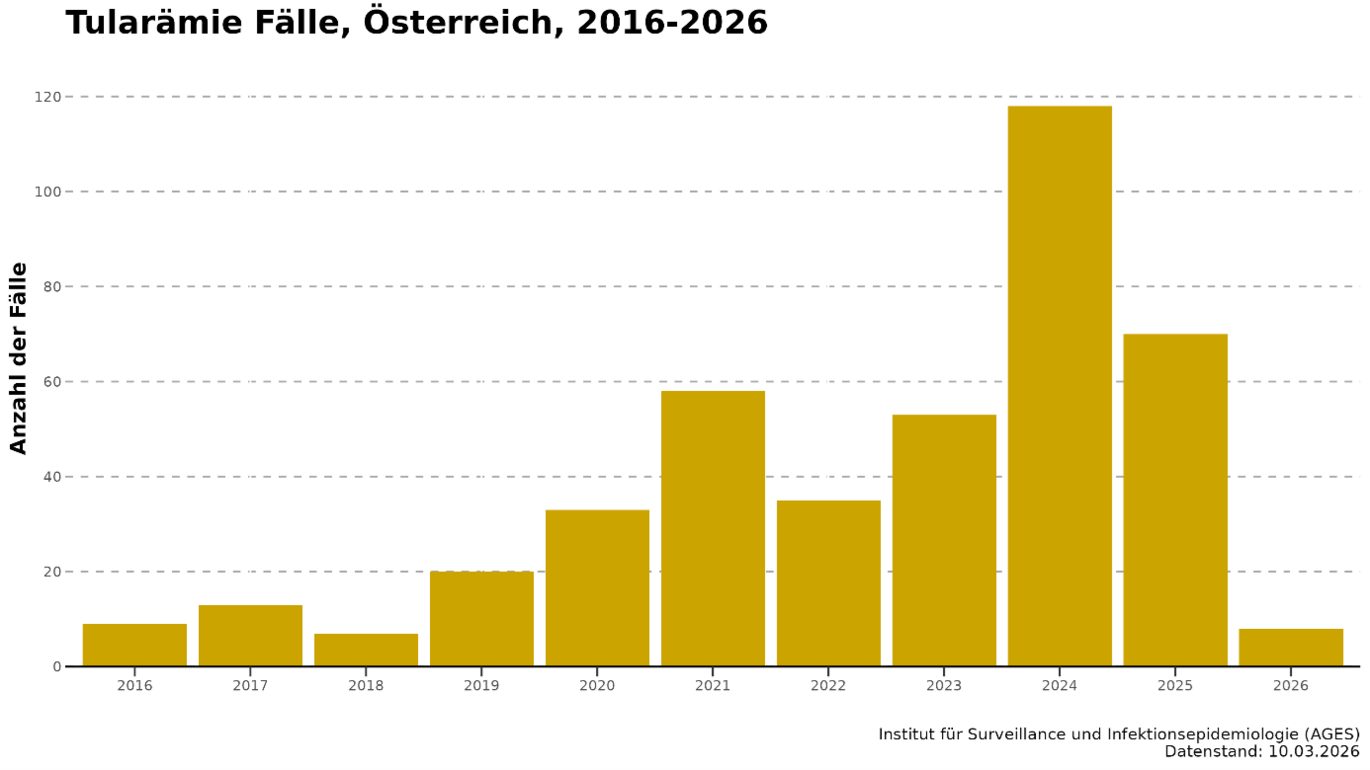
In recent years, a significant increase in reported cases of tularemia has been recorded in Austria (see Figure 1). Other European countries are also reporting rising case numbers. A specific cause for this increase in the disease has not yet been clearly identified. Factors under discussion include an increased detection rate due to more sensitive diagnostic methods, the effects of the climate crisis on the natural reservoirs, vectors and host animals of F. tularensis, as well as changes in personal behaviour (e.g. increased leisure activities in the countryside) associated with a higher risk of exposure.
The testing of brown hares for tularemia has a long history in Austria; cases were first identified as early as 1937 in central and southern Burgenland and the neighbouring Styria. This marked the start of sporadic testing, which was later followed by various projects. Since 2010, hares have been regularly sent for testing for tularemia when suspected of being infected, and positive cases are now also published on the AGES website. Human cases of the disease are recorded in the Epidemiological Reporting System (EMS). Many human cases in Austria can be traced back to contact with wild animals. However, a study conducted in 2022 by AGES colleagues, among others, shows that ticks have so far been underestimated as vectors of the disease. It describes three cases of bloodstream infections with F. tularensis in Austria that occurred following tick or insect bites (Heger et al., 2023). In fact, not much is yet known about the prevalence of F. tularensis in ticks in Austria. To gain a better overview of the situation, patients diagnosed with tularemia were therefore surveyed about insect or tick bites as part of the EU-funded United for Surveillance (U4S) project from 2023 to 2025. From the 40 questionnaires returned, it can be concluded that 18 had a history of tick bites. Furthermore, as part of the project, vectors were collected at 5 sites in Upper Austria and 3 in Lower Austria and tested for F. tularensis. The fieldwork took place at the locations where patients were most likely to have become infected with F. turalensis, and F. turalensis was detected in one tick.
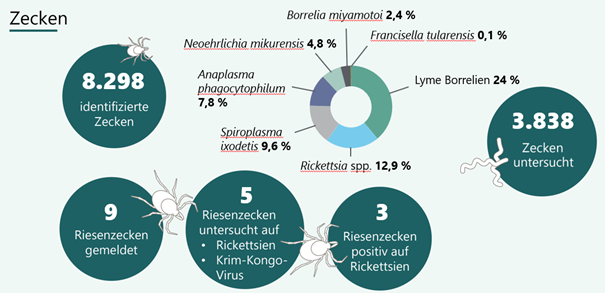
In the RAISE project, too, ticks sent in by citizen scientists have been tested for this pathogen since early 2025. Figure 2 illustrates, among other things, the proportion of pathogens found in the ticks examined. Of the 8,298 ticks submitted, 46% were tested for a range of pathogens. These included F. tularensis, which was found in 0.1%. Our results are therefore consistent with comparable international studies.
You can find all the latest results here: Tick Information – AGES.
Discovering ticks for research purposes
The citizen science project continues this year as the tick season gets underway, and we look forward to receiving tick submissions from all over Austria. Dead ticks can be easily sent by post to AGES, Department of Vector-borne Diseases, Währinger Straße 25a, 1090 Vienna. Live ticks can be handed in at a number of locations. You can find the exact addresses, details of what we do with the ticks, the results of all investigations, and lots of other useful tips and information about these cute arachnids here under Tick Information – AGES.
Sources:
Tularemia – WOAH – World Organisation for Animal Health
ECDC: Factsheet on tularaemia
BMG: Tularemia, https://www.verbrauchergesundheit.gv.at/dam/jcr:213432b6-a235-47d1-ba42-ff781ecfa552/BMG-74600_0201_2012_17_Merkblatt_Tularaemie__Aug2012.pdf
RKI Guide – Tularemia
AGES: Tularemia (rabbit fever)
Heger, F., Schindler, S., Pleininger, S., Fueszl, A., Blaschitz, M., Lippert, K., ... & Indra, A. (2023). Three cases of tick-borne Francisella tularensis infection, Austria, 2022. Emerging Infectious Diseases, 29(11), 2349. Detecting
ticks for research purposes – Austria Researches 2025
Tick Information – AGES
The 2025 annual report of the National Reference Centre for Pneumococci was published in February.
The national surveillance system monitors invasive pneumococcal disease (IPD) in Austria. In 2025, 944 cases of IPD were recorded, resulting in an incidence of 10.3 per 100,000 people.
The serotype could be determined in 880 of the registered IPE cases, with 41 different serotypes identified: serotype 3 (20.8%), serotype 19A (9.9%) and serotype 8 (8.3%) were detected most frequently.
Resistance testing against erythromycin, clindamycin, tetracycline, ceftriaxone and penicillin was carried out on 880 isolates. Of these, 11.5% of the isolates were resistant to erythromycin, 7.2% resistant to clindamycin and 8.3% resistant to tetracycline. In accordance with the guidelines of the European Committee on Antimicrobial Susceptibility Testing, the interpretation of penicillin or ceftriaxone resistance varies depending on the clinical presentation. With a minimum inhibitory concentration (MIC) breakpoint of ≤0.06 mg/L, 91.1% of the isolates would be considered fully susceptible to penicillin, and with an MIC of ≤0.5 mg/L, 99.4% would be considered fully susceptible to ceftriaxone.
In February, the 2024 annual report of the National Reference Centre for Legionella Infections was published.
In 2024, the National Reference Centre for Legionella Infections recorded 354 cases of Legionnaires’ disease, including 14 deaths. The upward trend observed over the past ten years thus continued in 2024. A clearly pronounced summer seasonality was again evident. The highest monthly incidence to date was recorded in September, at 0.71 cases per 100,000 inhabitants.
As in previous years, the majority of all 354 infections occurred among men in older age groups. The infections mainly took place in private settings. Only a small proportion (72 cases) could be attributed to travel and stays in accommodation establishments. Infections in healthcare facilities remain an exception, with six cases.
In 2024, 25 cases of Legionnaires’ disease in foreign tourists who had previously been in Austria were reported to the National Reference Centre by the European Legionnaires’ Disease Surveillance Network, the US Centres for Disease Control and Prevention, the Swiss Federal Office of Public Health and the UK Health Security Agency.
The Mosquito Alert Annual Report 2025 was published on 24 February.
Mosquito Alert collects information on the spread of non-native mosquito species whilst raising awareness of the health risks posed by mosquitoes. Citizens can use an app to submit photos of mosquitoes, which are then identified by experts.
In 2025, the number of reports continued to rise. The app is used particularly frequently in regions where tiger mosquito populations are already established: in Vienna and Styria. There are also increasing reports in Lower Austria and Upper Austria, although fewer sightings have been recorded there to date. Overall, the data show a significant spread of the tiger mosquito in Vienna, Graz and Linz compared to the previous year, 2024.
Denmark has eliminated mother-to-child transmission of HIV and syphilis – that is, before, during and after birth – and has been certified as such by the World Health Organisation (WHO). This makes Denmark the first EU country to achieve this health target and to have met all the criteria between 2021 and 2024. These include very low transmission rates (<50 per 100,000 births), high coverage of antenatal testing and adequate treatment for pregnant women. Crucial to this success were Denmark’s strong, well-developed and freely accessible healthcare system – particularly in primary care – as well as nationwide prevention programmes with screenings, robust laboratory capacities and an exemplary database system.
Denmark is now on the path to ‘triple elimination’ – the additional elimination of mother-to-child transmission of hepatitis B, which has so far been achieved in 22 countries and territories worldwide.
In January 2026, a dog imported from Russia was diagnosed with rabies in Germany after it had died. According to its vaccination certificate, the puppy in question had been vaccinated against rabies. Although documents indicated correct identification (microchip), a rabies vaccination and the required antibody titre, investigations following the animal’s death revealed discrepancies. According to these findings, the puppy was younger than originally stated. It is therefore currently assumed that an effective vaccination did not take place or that the vaccination record was falsified.
Other dogs were also being transported in the same vehicle as the infected dog. One dog went to new owners in Austria; the other dogs were handed over to new owners in Belgium, France and Switzerland. The Member States concerned were informed via the European notification system.
One of these contact dogs is currently in Vorarlberg. After the case came to light, the animal underwent a clinical examination and was placed under home quarantine. The two dog owners received active immunisation. The dog showed no symptoms during the observation period. A test at the AGES Mödling National Reference Laboratory revealed a sufficient antibody titre (0.66 IU/ml). A booster vaccination was administered after the end of the quarantine period. The dog remains clinically unremarkable.
Infection with the rabies virus is always fatal in both humans and animals. Therefore, medical care is urgently required if exposure to rabies is suspected. This case highlights the risk of rabies being introduced through the illegal trade in animals from regions where the disease is still present. Suspected cases, confirmed cases and fatalities, as well as bite injuries caused by rabid or suspected rabid animals, are subject to mandatory reporting and must be reported to the district administrative authority within 24 hours. Further information on purchasing animals from abroad and what to bear in mind can be found on the website of the Federal Ministry of Labour, Social Affairs, Health, Care and Consumer Protection.
Terrestrial rabies, i.e. ‘land-based rabies’, transmitted by ground-dwelling mammals such as foxes, dogs, etc., has been eradicated in Austria since 2008. The WHO has certified Austria as rabies-free. This also applies to all neighbouring countries. Bat rabies must be distinguished from terrestrial rabies; it was first confirmed in Austria in September 2023 in a dead bat. Transmission via bats cannot therefore be completely ruled out, even though it has never been observed in Austria.
Caution when buying animals from abroad: Recent rabies case in Germany highlights risks Latest
news on rabies in Germany | Friedrich-Loeffler-Institut
Animal welfare abroad carries risks: Rabies case raises alarm / German Veterinary Association
26/02/26 – Germany: Fatal rabies case in imported animal
AGES – Rabies
In March 2026, Chile was officially certified as free of leprosy by the WHO and the Pan American Health Organization (PAHO). This makes Chile the first country in the Americas and the second in the world, after Jordan (2024), to have this elimination – that is, the cessation of leprosy transmission within its national territory – confirmed.
Historically, leprosy in Chile occurred primarily on Easter Island, whilst only a few cases were recorded on the mainland. The last locally transmitted case was reported in 1993. Between 2012 and 2023, Chile reported 47 cases, all of which were imported. Nevertheless, leprosy remained a notifiable disease and was monitored through integrated surveillance. Leprosy frequently affects population groups living in vulnerable conditions. According to the WHO, early diagnosis, universal access to treatment and continuous epidemiological surveillance have contributed significantly to its elimination. This underscores the need to keep an eye on even rare infectious diseases and the importance of concentrated efforts in the fight against infectious diseases.
We have covered more on leprosy and the associated stigma in the “Topic of the Month” section of the AGES-Radar issue dated 22 January 2026.
The AGES Infectious Diseases Radar is published monthly. Its aim is to provide Austrian health services and the interested public with a quick overview of current infectious diseases in Austria and around the world. The diseases are briefly described, the current situation is outlined and, where appropriate and possible, the risk is assessed. Links provide further information. The ‘Topic of the Month’ section examines one aspect of infectious diseases in greater detail.
How is the AGES Radar for Infectious Diseases produced?
Who: The Radar is a collaboration between the AGES departments of “Public Health”, Knowledge Management and Risk Communication.
What: Outbreaks and situation assessments of infectious diseases:
- National: Based on data from the Epidemiological Reporting System (EMS), outbreak investigations and regular reports from AGES and the reference laboratories
- International: Based on structured research
- Topic of the month (annual planning)
- News on scientific publications and events
Further sources:
Acute infectious respiratory diseases occur more frequently during the cold season, including COVID-19, influenza and RSV. These diseases are monitored via various systems, such as the Austrian Influenza Diagnostic Network (DINÖ), the ILI (influenza-like illness) sentinel system and the Austrian RSV Network (ÖRSN). The situation in hospitals is monitored via the SARI (Severe Acute Respiratory Illness) dashboard.
For international reports, health organisations (WHO, ECDC, CDC, etc.), specialist media, the international press, newsletters and social media are routinely monitored.
For infectious diseases in Austria, the situation is assessed by AGES experts; the same applies to international outbreaks for which no assessment is available from the WHO or ECDC.
Disclaimer: Topics are selected according to editorial criteria; no claim is made to completeness.
Suggestions and questions to: wima@ages.at
As responses to enquiries are also coordinated among all parties involved (Knowledge Management, MED, Risk Communication), we ask for your patience. A response will be provided within a week.
Case numbers for notifiable diseases under the Epidemics Act; the figures shown are for the previous month and, for the period from the start of the year to the end of the previous month, the figures for the current year, the previous year, and the median of the last five years for comparison (Epidemiological Reporting System, as at 11 March 2026).
a Diseases are assessed in accordance with the case definition. Diseases for which a case definition exists are shown, with the exception of transmissible spongiform encephalopathies. As a rule, confirmed and probable cases are counted. Changes may still occur due to late reporting or subsequent entries.
b Bacterial and viral food poisoning, in accordance with the Epidemics Act.
c Invasive bacterial disease, in accordance with the Epidemics Act.
d Includes only cases involving pneumonia.
e Due to the lack of a case definition prior to 2025, only cases from 2025 onwards are shown; the median is also calculated only from 2025 onwards.
f Mpox has been a notifiable disease since 2022; the median is calculated only for the years in which it is a notifiable disease.
Last updated: 22.05.2026
automatically translated